For millions grappling with excruciating pelvic pain, the path to an endometriosis diagnosis and subsequent surgical intervention often spans a heartbreaking decade or more. This prolonged suffering, frequently dismissed as 'normal period pain,' highlights a critical gap in women's health awareness, medical education, and accessible specialist care. Understanding the complexities of endometriosis and the challenges in obtaining timely treatment is crucial for both patients and healthcare providers.
The Labyrinth of Endometriosis Diagnosis
Endometriosis is a chronic condition where tissue similar to the lining inside the uterus (the endometrium) grows outside of it. These growths, known as implants, can be found on ovaries, fallopian tubes, the outer surface of the uterus, and even on the bowel or bladder. Like the uterine lining, these implants respond to hormonal changes, thickening, breaking down, and bleeding during the menstrual cycle. However, unlike menstrual blood, this blood has nowhere to go, leading to inflammation, pain, scar tissue, and adhesions that can bind organs together.
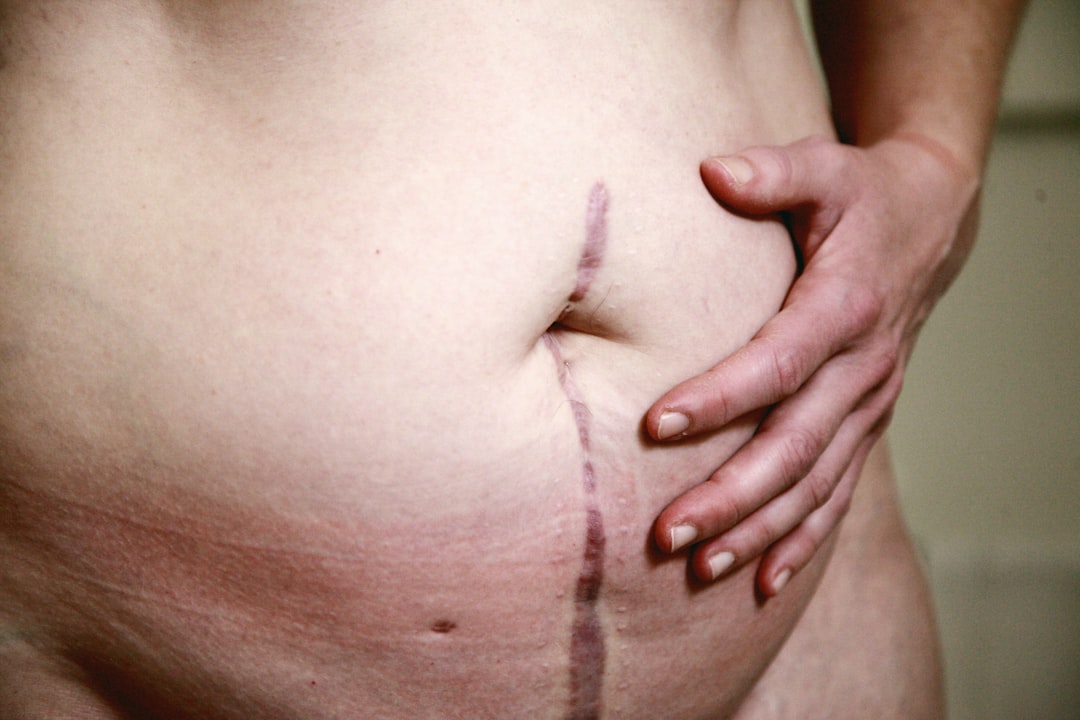
Understanding Endometriosis: What It Is and Its Manifestations
The severity of endometriosis doesn't always correlate with the intensity of pain; some individuals with extensive disease experience minimal discomfort, while others with mild cases endure incapacitating agony. Common symptoms extend far beyond just painful periods, encompassing chronic pelvic pain, pain during or after sex (dyspareunia), heavy or irregular bleeding, fatigue, painful bowel movements or urination, and infertility. These diverse and often debilitating symptoms can significantly impact daily life, relationships, and professional productivity.
Why the Diagnostic Delay Persists
The average diagnostic delay for endometriosis globally is estimated to be between 7 and 10 years, a statistic that has remained largely unchanged for decades. Several factors contribute to this staggering wait. Firstly, there's a pervasive societal normalization of women's pain, particularly menstrual pain, leading many individuals and even some medical professionals to believe severe discomfort is an inevitable part of menstruation. Secondly, endometriosis symptoms often mimic those of other conditions, such as irritable bowel syndrome (IBS), pelvic inflammatory disease (PID), or ovarian cysts, making accurate differentiation challenging. Thirdly, the definitive diagnosis of endometriosis traditionally requires a laparoscopic surgical procedure, which is invasive and not always the first line of investigation. Finally, a general lack of awareness and specialized training among some primary care physicians regarding the nuances of endometriosis can lead to misdiagnosis or delayed referrals to specialists.
The Profound Impact of Chronic Pain and Delayed Care
Living with undiagnosed or untreated endometriosis for years inflicts a tremendous toll, not just physically but also mentally, emotionally, and socio-economically. The relentless nature of chronic pain wears down resilience, affecting every facet of an individual's existence.
The Physical and Emotional Burden
Beyond the direct pain, chronic inflammation and scarring can lead to further complications, including ovarian cysts (endometriomas), severe adhesions that distort pelvic anatomy, and potential involvement of bowel or bladder, causing gastrointestinal or urinary symptoms. The constant fight against pain and fatigue often leads to significant mental health challenges, with higher rates of depression, anxiety, and feelings of isolation reported among those with endometriosis. The inability to participate fully in social activities, maintain consistent employment, or even perform basic daily tasks can erode self-esteem and quality of life.
Impact on Fertility and Quality of Life
Endometriosis is a leading cause of infertility, affecting up to 50% of women struggling to conceive. The presence of endometrial tissue can disrupt ovulation, impede the movement of eggs and sperm, and create an inflammatory environment hostile to pregnancy. Even for those who do not desire children, the condition's impact on sexual health, energy levels, and overall well-being can be devastating, leading to relationship strain and a diminished sense of control over one's body and future.
Navigating Treatment: When Surgical Intervention Becomes Essential
While various treatments aim to manage endometriosis symptoms, surgical intervention, particularly excision surgery, is often considered the gold standard for definitive diagnosis and removal of endometrial implants, offering the best chance for long-term relief.
From Symptom Management to Definitive Treatment
Initial treatment strategies often focus on pain management through over-the-counter or prescription painkillers and hormonal therapies. Hormonal treatments, such as birth control pills, GnRH agonists, or progestins, work by suppressing the menstrual cycle and reducing the growth of endometrial tissue. While these can alleviate symptoms for some, they do not eradicate the disease and symptoms often return upon discontinuation. For many, especially those with severe pain, extensive disease, or fertility issues, surgery becomes a necessary and often life-changing step.
The Role of Laparoscopic Excision Surgery
Laparoscopic surgery, a minimally invasive procedure, serves both diagnostic and therapeutic purposes. During laparoscopy, a surgeon makes small incisions to insert a camera and specialized instruments, allowing them to visualize and remove endometrial implants. Excision surgery, where the implants are carefully cut out from their roots, is generally preferred over ablation (burning the surface), as it aims to remove the entire lesion, reducing recurrence rates and providing more comprehensive relief. The journey to obtaining this specialized surgery often requires persistent advocacy, multiple consultations, and referral to an endometriosis specialist.
Empowering Your Journey: Advocacy and Support
Given the complexities of endometriosis and the persistent diagnostic delays, patient advocacy plays a crucial role in securing timely and effective care. Understanding how to navigate the healthcare system and connect with appropriate resources can make a significant difference.
Speaking Up and Finding the Right Specialists
Individuals experiencing persistent pelvic pain should meticulously track their symptoms, noting their intensity, duration, and any aggravating or alleviating factors. This detailed information can be invaluable when consulting healthcare providers. It is essential to be assertive in seeking answers and not hesitate to get second or even third opinions if concerns are dismissed. Identifying and consulting with an endometriosis specialist – a gynecologist with advanced training in diagnosing and surgically treating the condition – is paramount. These specialists possess the expertise to recognize subtle signs, perform advanced surgical techniques, and develop comprehensive management plans.
Community, Research, and Future Hope
Connecting with support groups and patient communities can provide invaluable emotional support, shared experiences, and practical advice on navigating the condition. Organizations dedicated to endometriosis research and advocacy are continuously working to raise public awareness, improve diagnostic tools, and accelerate the development of new treatments. The collective efforts of patients, advocates, and researchers offer hope for a future where endometriosis is diagnosed much earlier, and effective, accessible treatments are readily available, sparing individuals years of debilitating pain and suffering.






